
By Jemma Hatton, Senior Audiologist
Most tinnitus specialists are audiologists who have undertaken further training in tinnitus therapy. One of the most common aspects of work when delivering adult rehabilitation in audiology is working with elderly patients. However, one of the enjoyable things about delivering tinnitus therapy is working with patients from a wider demographic, including working adults. These patients present different challenges and their priorities may differ from those in an older demographic. In my experience working adults also tend to have greater access to resources and other evidence to discuss their treatment in depth.
The access to further resources can be an interesting challenge when there currently no cure for tinnitus. For many tinnitus patients, a perfect scenario would be for their tinnitus to be removed entirely. However, when presented with the idea of Cognitive Behavioural Therapy (CBT), a form of counselling which could be effective in managing their tinnitus, this can often have mixed responses. Working adults often worry about not being able to concentrate at work and having no opportunity to wind down at the end of the day as their tinnitus remains present. CBT takes time and effort which can be frustrating for a working adult with limited time as opposed to taking a medicine which is perceived as providing a quicker means of treatment for many medical conditions. This can be a tricky expectation to address. It is also common that these patients have reservations about displaying their vulnerabilities and sharing their deepest worries and fears. These patients can be concerned that by disclosing this information to a stranger, that this can show weakness in their character and capability at work and in supporting their families.
Case Study

I started the care for Jonathan (pseudonym) in summer 2021. Jonathan was aged 43 and had been referred to the service by an ENT consultant. He attended his tinnitus assessment and described continuous hissing in the left ear which had been present for six months. A hearing test had been completed which had revealed normal hearing and the ENT investigations were unable to identify any specific cause for the onset of his tinnitus. He presented with no history of mental health concerns and the mental health screening checks suggested no symptoms of anxiety or depression. The main impact the tinnitus was having was being unable to relax in the evenings. I presented the idea to Jonathan of CBT and how this could benefit him. Jonathan’s initial response was hesitancy as whilst he had been informed there was no cure, I sensed he had been hoping I would tell him something differently at the assessment. He had never received counselling before and it took some time for me to explain how his emotional response could be impacting his management of his tinnitus. He asked about other options including changing his diet and taking medication. I explained these weren’t suitable to help him overcome the issues around managing his tinnitus so he reluctantly agreed to proceed and attend another appointment to commence his CBT.
A couple of weeks later Jonathan came back to the clinic to attend his first CBT session. I started off by getting to know Jonathan and trying to understand what it was like to be in Jonathan’s shoes and how his life was affected by tinnitus. He explained to me he worked as a project manager and had recently started a new job having been made redundant from his previous employer. The new job was generally going well however he noted it could be quite pressurised and stressful therefore downtime at home is important to him. He was also very conscious of the recent redundancy and reported he always had this in the back of his mind.
He had a family including a wife and children to support and spending quality time with them outside work was particularly important to him to maintain his relationships with his family. He reported that he is a natural worrier and being able to relax following a stressful day at work was crucial to him feeling generally well in himself. The primary impact of his tinnitus was he was struggling to relax in the evening particularly whilst watching TV. He would overcome this by often staying busy in the evening and avoiding this activity, so he didn’t notice his tinnitus. He reported that he had no concerns with sleep as he was generally exhausted by bedtime, and he didn’t notice his tinnitus much at work as he was so busy. His primary goal from the treatment was to be able to relax when tinnitus is present.
We explored his tinnitus related distress further by completing a formulation which is a model where we identify the thoughts, feelings and emotions associated with tinnitus. We based this on him watching TV the night before and then him hearing his tinnitus. His initial thoughts were as follows;
This was accompanied by the emotions: sadness, annoyance and upset
We then explored further and identified the following evaluative thoughts;
I presented the formulation to the patient and showed him how his thoughts and emotions were linked to his tinnitus. He had a much better understanding of how his thoughts were affecting his emotional response to tinnitus. He went away and reflected on this. When he came back for his next appointment, he had a fresher perspective on his tinnitus and was keen to start getting involved with some CBT interventions.
The first intervention we did was a behavioural experiment; an opportunity to test if his thoughts really were true. We decided he would watch TV with his family and he wouldn’t be able to start doing lots of activities to keep himself busy to distract him from his tinnitus. He was open-minded to undertake this and keen to proceed to see the outcome.

He returned the next week for a further session having following completing the experiment and was delighted that the experiment had gone much better than he had expected! We discussed the outcome of this and used the information to create some alternative thoughts (counter-statements) to help him manage his tinnitus. As the clinician I asked many questions to ensure Jonathan was confident with the counter-statements and truly believed them. The counterstatements were as follows:
At the end of this experiment, I asked Jonathan to complete a diary of thoughts and feelings for the next appointment to help to identify any further situations with tinnitus related distress. He came back the following week with the completed diary. He had identified a few situations on a family day out over the previous weekend and in some meetings which at work which he found boring. We created the following counter-statements to help him manage his tinnitus following this additional information;
I asked Jonathan to create the diary once more for the final appointment, however I wanted him to fill in the counterstatements himself to demonstrate he understood CBT. The next week he returned with the diary, in which he hadn’t noted many situations with tinnitus related-distress as he felt he was coping much better and was more confident creating his own counterstatements. He recognised he understood how to prevent the negative spiral that affected his tinnitus-related distress and felt confident in managing this independently. This was reflected in his outcome measurements which can be seen in the table below:
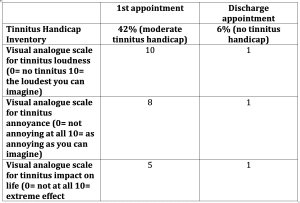
As can be seen from the table, through Jonathan changing his mindset from being a reluctant patient to a patient fully engaged in CBT and proactive with his assignments, it clearly resulted in a significant improvement of his quality of life. Jonathan no longer found that tinnitus dominated his relaxation time during evenings and weekends. He believed he could enjoy his life with tinnitus and was now able to unwind from his job with ease. To lean more about tinnitus and its treatment click here.